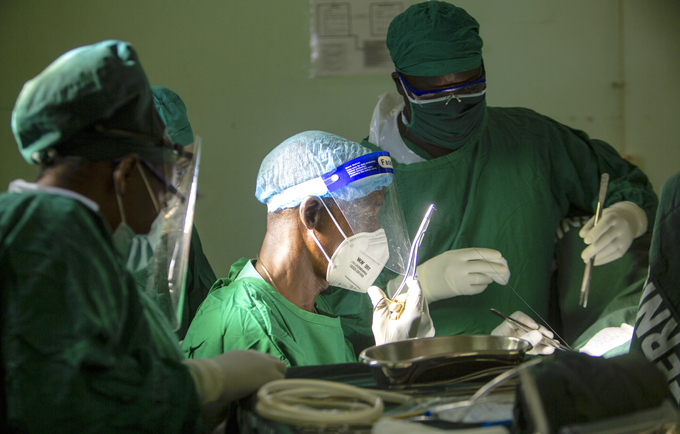
Obstetric fistula is almost entirely preventable, its persistence a sign that health systems are failing to meet women’s essential needs. A fistula forms as the direct result of obstructed labour, one of the major causes of maternal deaths. This is where the mother’s pelvis is too small for the baby to be delivered without help. Obstetric fistula happens during a long and obstructed labour. The pressure caused by the obstructed labour damages the tissue of the internal passages of the bladder and/or rectum. With no access to a Caesarian section and emergency obstetric care, the woman may be left permanently incontinent. This means being unable to hold urine or faeces, which leak out through her vagina. In about 90 per cent of cases, the baby does not survive, which means the mother has to deal with the devastating internal injuries on top of losing her baby.
A fistula can usually be repaired with reconstructive surgery. Most women affected by this injury do not know about the treatment available, however, or they are unable to afford it or to reach the facilities where it is available. Once a woman has been treated, she may also need counselling and skills training to help her reintegrate into her community.
The causes of fistula
The physical causes are limited access to health care, including essential obstetric care during pregnancy and childbirth, adolescent fertility (early marriage), and existing harmful practices such as female genital mutilation, which affect the normal delivery process.
Obstetric fistula is still increasing because health systems fail to provide essential and emergency obstetric care during pregnancy and childbirth, including family planning and the affordable treatment of fistula.
The poor integration of sexual and reproductive health (SRH) services for adolescents and comprehensive SRH packages into existing national health systems also contributes to fistula. Young couples need opportunities to postpone their first pregnancy, avoid early pregnancy and space births.
The key to ending fistula is prevention. This entails ensuring that all women have access skilled birth attendants and emergency obstetric care if they develop complications during delivery. Additionally, the provision of family planning to those who want it could reduce maternal disability and death by at least 20 per cent.
UNFPA’s response
UNFPA and its partners launched the Global Campaign to End Fistula in 2003 to redress the unacceptable human rights and equity dimensions of obstetric fistula. Since the campaign started, UNFPA has helped many women and girls access fistula treatment and care.
Thousands of women and girls have also received reintegration services, including psychological support, skills training and small grants to start businesses with support from the Maternal and Newborn Health Thematic Fund. UNFPA has also supported the training of thousands of health workers, including surgeons, midwives, nurses and community health workers. These health professionals all play a crucial role in treating fistula, preventing its occurrence, identifying survivors and referring them to care.
In 2016, on International Day to End Obstetric Fistula, UN Secretary-General Ban Ki-moon called upon the world to end fistula within a generation, a message reiterated by UNFPA's Executive Director. In December 2018 and 2020, Member States adopted a UN resolution on fistula, calling for an end to fistula within a decade, in line with the 2030 Agenda for Sustainable Development.
This bold vision raises the bar for addressing fistula, putting it on the same level as other major global initiatives including ending preventable maternal and newborn deaths, ending HIV, ending female genital mutilation and eradicating polio.
In 2021, UNFPA and the Campaign to End Fistula released a new edition of the global UN guidance, Obstetric Fistula & Other Forms of Female Genital Fistula: Guiding principles for clinical management and programme development. With the latest evidence, strategies, tools and resources, the manual shows the global/UN vision of the new way forward and paradigm shift in approaches towards eradicating fistula by 2030.