When Sarah Nyirangirimana, 33, became pregnant with her second child four years ago, she felt enthusiastic about the pregnancy, which had occurred almost 11 years after her first child was born.
“I was the happiest woman on earth! I was looking forward to giving birth to a child I considered a gift from God,” she said at Kyeshero hospital in Goma, North Kivu province, in the Democratic Republic of Congo (DRC).

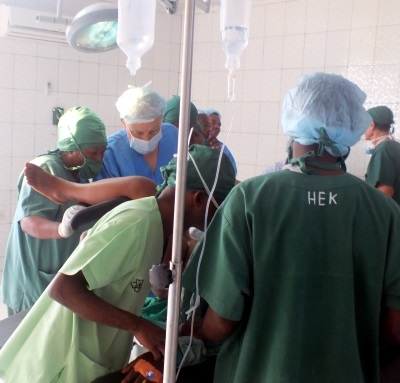
Sarah was one of 100 women with complex obstetric fistula who had gathered at the hospital to undergo surgical repair, with the assistance of Congolese and foreign surgeons UNFPA had brought together for a three-week fistula repair campaign. This was organized in partnership with the DRC Ministry of Health in the provinces of Kinshasa, North Kivu and Haut Katanga.
Sadly, the pregnancy that initially brought Sarah so much joy also marked the beginning of an horrific ordeal.
Due to fighting between the Armed Forces of the Democratic Republic of Congo (FARDC) and the M-23 (Mouvement du 23 mars) rebel armed group in the mountainous territory of Rutshuru, around 30 kilometres North of Goma, where she lived, Sarah could not access a health facility even for prenatal care.
“Roads were blocked or unsafe and it was difficult to move around. We women were bearing the brunt of the violence, with rape, abductions, shooting and looting (going on) throughout the area,” she said from her bed in the waiting room of Kyeshero hospital.
The security situation in Rutshuru in those days was alarming, as members of the armed groups involved in the conflict frequently raped women as a means of intimidation, with the risk of unwanted pregnancies, miscarriages and sexually transmitted infections. This led to school children avoiding school for fear of being attacked and forced to fight. It also led to the displacement of people inside North Kivu or to neighbouring countries. At one point, the Congolese Government no longer controlled the town of Rutshuru, which became a stronghold of the M-23 rebel group.
It was painful. Only family members who did not have any medical background attended to me. - Sarah Nyirangirimana, fistula survivor
Sarah carried her pregnancy to term despite these difficult circumstances and after many hours of labour without any medical help, she gave birth to a stillborn boy.
“It was painful. Only family members who did not have any medical background attended to me,” she recalled. Then, days after the delivery, she found that she could no longer control the flow of urine.
Her incontinence was unbearable and she felt ashamed. When the security situation normalized and Rutshuru was returned to the Congolese armed forces after more than a year under the control of M-23, she rushed to Rutshuru General Hospital to seek help for her medical condition. There, she learnt that the unattended labour had left her with a fistula and that she needed to undergo surgery if she wanted to be cured.
“That was the first time I had heard of fistula. I was willing to undergo surgery to regain my dignity, because everybody was mocking me and running away from me,” she declared.
But four years and four unsuccessful surgeries later, Sarah remained incontinent. This was why she found herself sitting with 22 other women in the waiting room at Kyeshero hospital, anticipating her fifth operation. Most of these women had, like her, undergone numerous unsuccessful surgeries.
It is our duty to ensure that all cases, no matter how complicated they are, are examined and treated, as our goal is to end fistula. - Diene Keita, UNFPA's Representative in the DRC
Complex cases like theirs resulting in numerous failed operations were the reason that UNFPA DRC had brought together surgeons from France, Senegal and the DRC, not only to attempt to repair them successfully, but also to share experiences, and transfer knowledge and competency for better results, said Dr. Magueye Gueye, the Senegalese member of the team performing the surgeries.
For Diene Keita, UNFPA's Representative in the DRC, no women suffering from fistula should be left behind. “It is our duty to ensure that all cases, no matter how complicated they are, are examined and treated, as our goal is to end fistula,” she said. Around 100 women in the cities of Kinshasa, Goma and Lubumbashi were to undergo surgery during the campaign .

Another member of the surgery team, Professor Ludovic Falandry from France, who had been dealing with fistula cases since 1978, recognizes that unsuccessful operations are common. “That is the worst thing that can happen to the campaign to end fistula, as for every failure, all other women suffering from fistula in the same village as the woman with the unsuccessful surgery, are lost to us. They will never show up for surgery and that is why we must do our utmost to succeed,” he declared.
For Professor Manga Okenge of the University of Kisangani, a fistula surgeon for more than 20 years, this experience of sharing knowledge and competency transfer should be encouraged everywhere, as it allows surgeons to learn from each other, to train those less experienced, and to deal with complex cases like Sarah’s.
Professor Manga, who developed a reputation as the doctor who performed surgeries with a razor blade under candlelight, said that while training is important in dealing with fistula, on its own it is not sufficient. Practice, patience, humility to learn from others and commitment to save lives were important as well, he said. Asked about his reputation, he admitted with a smile that this was in the darkest days of the country, when the war was still raging. “When you take that oath, you have to do what needs to be done to save lives by any means necessary," he said.
The campaign itself was about allowing Sarah and other fistula patients like her to reclaim their dignity, said Dr. Felix Kabange Numbi, the DRC Minister of Health.
As for Sarah, she remained under observation in the hospital three weeks after her surgery, with the hope of returning home fistula free and her smile regained.
By Assane Ba



